The Virtual reality: applications, mechanisms, and rehabilitation implications: a narrative review
DOI:
https://doi.org/10.52567/trehabj.v9i04.116Keywords:
cerebral palsy, neurological deficits, rehabilitation, stroke, virtual realityAbstract
Background: Virtual Reality (VR) is an emerging technology that creates immersive, interactive environments, offering real-time feedback, task-specific repetitive practice, and gamified exercises that enhance neuroplasticity, motivation, and adherence during rehabilitation.
Objective: To synthesize current literature on VR applications, mechanisms of action, and rehabilitation outcomes across diverse populations.
Methodology: A comprehensive literature search was conducted in Google Scholar, PubMed, Elsevier, and JSTOR for studies published between 2015 and 2024. Randomized controlled trials, quasi-experimental trials, pilot studies, systematic reviews, and meta-analyses using VR as a primary intervention in rehabilitation were included in the review. Data were extracted on study design, sample characteristics, type of VR intervention, duration, and motor or functional outcomes. Twelve studies meeting inclusion criteria were synthesized narratively, highlighting intervention types, effects, and trends across patient populations.
Results: VR-based interventions demonstrated significant improvements on upper and lower limb motor function, gait, balance, and independence in post-stroke patients. While the Parkinson’s patients exhibited enhanced postural control, gait, and reduced fall risk. Intensive VR-based exergaming showed great improvement in gross motor function and coordination as well as engagement and motivation in children with cerebral palsy. In older adults’ VR improved balance, dual-task walking, and functional mobility. High satisfaction and tolerability were indicated as patients reported consistent improved outcomes. Despite these benefits, low awareness, training gaps, and equipment costs have reduced its adoption in clinical settings. Low cost VR solutions can be safely employed in resource-limited clinical settings as suggested by feasibility studies.
Conclusion: Motor recovery, neuroplasticity as well as patient engagement are greatly improved with use of VR based therapy as it is a promising adjunct to traditional exercises and conventional rehabilitation.
INTRODUCTION
Virtual reality (VR) is a technology that creates immersive, interactive 3-D environments by simulating real or imagined worlds [1]. In rehabilitation, movements and activities of daily living can now be practised in safe, controlled, and engaging virtual settings [2, 3]. Recent advances in VR such as affordable head-mounted displays, motion-capture sensors, and integration with telemedicine and AI - have greatly expanded its use in healthcare and physiotherapy [2, 4]. Home and clinics now have easy access to VR due to recent developments. The ability to precise tracking and feedback on patient performance has enhanced [4].
The gamified and task-oriented exercises through VR has strongly enhanced motor learning and coordination. VR accelerates motor skill acquisition more effectively than conventional therapy by providing real-time visual and haptic feedback on movement. Various systematic reviews have reported that intensive, repetitive practice with immediate performance feedback through VR-rehabilitation, drive neuroplasticity and skill retention [3, 5]. VR environments can be tailored and adjusted to specific patient’s ability level, thus increasing engagement and motivation during therapy [3, 4]. Importantly, VR training stimulates synaptic plasticity in the brain by activating neural circuits associated with reward and motor planning, thereby stimulating synaptic plasticity in the brain [2, 5].
VR interventions which are fully-immersive have shown significant effect across various patient populations. VR training improved upper-limb functions, gait, balance, and independence, with improved motor skills to real-world tasks in post-stroke rehabilitation [3, 6]. Among Parkinson patients, VR-based balance and gait exercises, have improved the postural control, walking ability, and reduced fall risk. This also stimulated automatic motor pathways and cognitive processes [3, 5]. VR modifies therapy as engaging and less fatiguing. Intensive training showed positive improvements in gross motor skills and coordination in the upper limb function in CP children [7]. Among older adults, VR-based exercise programs showed improvements in gait speed, dual-task walking, and overall mobility. Reduction in fall-risk markers and dual-task costs were also noted. The older adults achieved safer and more confident ambulation [8].
Due to lack of awareness and training in VR, it is still under-utilized and less explored in many clinical settings [9]. High quality VR requires costly reliable hardware and sometimes custom software, creating technical hurdles [4]. There are also limited clinical guidelines for VR integration, and concerns related to patient safety. Collectively, these issues and barriers contributed in lack of use of VR in rehabilitation practice.
Hence an updated narrative review is needed as the VR technologies are undergoing rapid evolution and the evidence base is growing. Such as low-cost and high-end systems, clarify the underlying mechanisms of examine the feasibility for implementation of VR in resource-limited clinical settings. As healthcare systems strive to expand rehabilitation access worldwide, it is crucial to highlight potential of VR as well as its limitations in low-resource contexts. By covering the latest innovations, outcomes, and real-world challenges, this review aims to guide clinicians and policymakers on harnessing VR’s full promise in rehabilitation.
METHODOLOGY
Study Design: For this narrative review the Scale for the Assessment of Narrative Review Articles (SANRA) guidelines was used, in the study to be transparent, comprehensive, and methodologically sound accuracy. The objective was to summarize the literature on Virtual Reality (VR) as an intervention in rehabilitation settings.
Search Strategy: To conduct a comprehensive literature search the Google Scholar, PubMed, Elsevier, and JSTOR were used. The main focus of the search strategy was to explore the studies using VR in rehabilitative interventions, published between 2015 and 2024. The virtual reality, cerebral palsy, stroke, neurological deficits, motor declines, healthy older adults, and community dwelling individuals were the keywords used for literature search by applying Boolean operators (AND, OR) to refine the search results. The reference lists of relevant articles were also screened to identify the more studies.
Inclusion and Exclusion Criteria: The studies included in this review are the pilot studies, randomized controlled trials, quasi experimental, systematic reviews and meta-analysis conducted on human participants in which primary intervention was the VR in healthcare or rehabilitation. The studies lacking a clear methodological description, focusing primarily on teacher, parent, or caregiver perspectives rather than participant outcomes, were excluded.
Study Selection: Following the screening of databases and abstract review of the articles, a total of n=12 meeting the inclusion criteria were selected for synthesis. A range of research designs represented in the selected articles were the randomized controlled trials, quasi-experimental trials, pilot studies, systematic reviews, and meta-analyses.
Data Extraction and Synthesis: Data were extracted on the study designs, sample characteristics, types of VR intervention, duration, and outcomes related to motor and functional performance. There was no statistical method was used for data collection but narratively synthesized to highlight the trends, similarities, and variations among studies. Several studies have consistently shown that virtual reality can be a valuable tool in rehabilitation. Various VR platforms were included used in previous researches, such as Nintendo Wii, Microsoft Kinect, Mandala Gesture Xtreme, and PlayStation-based systems. The duration of VR programs varied widely, from 10-minute sessions to several weeks, showing that these interventions can be easily adapted for different age groups and rehabilitation settings.
RESULTS
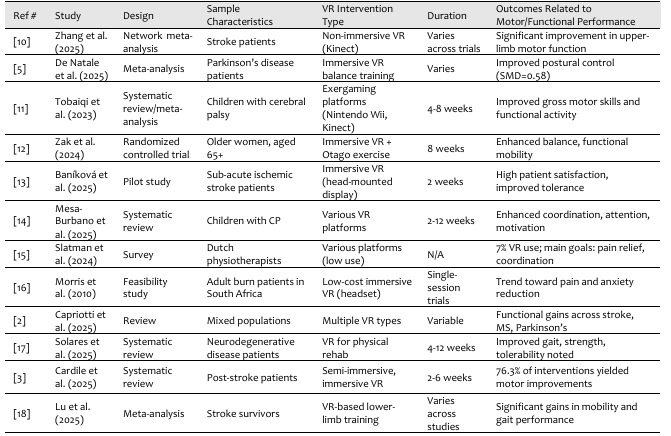
The narrative summery table of n=12 studies highlighting the main results, study features, types of VR interventions, their duration, and the functional outcomes reported. It also shows the current trends; VR effectiveness and approaches can be applied in clinical practice.
Table 1: Overview of VR Interventions and Outcomes
DSCUSSION
The current study’s objective was to synthesize current literature on VR applications, mechanisms of action, and rehabilitation outcomes across diverse populations, and also examined barriers to clinical adoption and feasibility in low-resource settings. Recent evidence strongly supports the efficacy of VR-based rehabilitation across a variety of conditions. Combined immersive VR and conventional therapy significantly improved postural balance in Parkinson’s disease, compared to conventional therapy alone, as investigated in a meta-analysis conducted in 2025 [5]. Similarly, in stroke recovery, non-immersive VR (using devices like the Microsoft Kinect) was the most effective modality for improving upper limb motor function as reported in a systematic review (2025) [10]. Another meta-analysis showed that VR-based exercise substantially enhanced lower-limb mobility after stroke [18]. A review also noted that the majority of VR interventions (76.3%) produced positive motor outcomes among post-stroke patients, with semi-immersive systems yielding the highest proportion of improvements. These findings indicate that VR can be an effective adjunct to standard therapy for neurological conditions, engaging patients with motivating, task specific exercises and potentially facilitating neuroplasticity [3].
Virtual reality is also being applied in pediatric and geriatric rehabilitation. In children with cerebral palsy (CP), systematic reviews have found that VR interventions lead to improvements in gross motor function, balance, and upper limb coordination, while also increasing engagement and motivation [14]. One systematic review and meta-analysis specifically reported that VR-assisted exergaming produced significant improvement in motor skills for children with CP [11]. Among older adults, the studies also encouraged that a fully immersive VR exercise program combined with dual-task cognitive components significantly improved balance in older women, beyond what was achieved with conventional Otago exercises [12]. In general, these studies reported that participants perceived VR-based exercises as enjoyable as and less burdensome than traditional therapy, and outcomes often included measurable gains in strength, coordination, and functional mobility [3, 12, 14].
Patient reported positive outcomes on VR rehabilitation in a pilot study of subacute stroke patients, with very high levels (68%) of satisfaction and tolerability with VR therapy. Patients rated clarity of information and perceived therapeutic benefits [13]. These findings align with other reports that VR’s immersive and interactive nature tends to enhance motivation and engagement during therapy.
There is a limitation in definite adoption of VR in clinical settings, despite having immense potential. Only about 7% primary care physiotherapists had integrated VR into treatment for chronic pain conditions in a survey conducted in Netherlands recently. Those who primarily used VR for lessening pain and enhancing coordination, rated their experience moderately positive. A very small percentage of physiotherapists have adopted VR since the past two years [15]. Deficiency of familiarity and training with the technology as well as restricted resources became the major barriers to wider use of VR. Increased engagement of VR in clinical practice could be augmented through rigorous training and evidence.
In resource-limited settings, low-cost VR can be feasible and beneficial as shown in various pilot studies. A feasibility trial conducted in South Africa used an inexpensive head-mounted display during physiotherapy for adult burn patients. Although, statistically significant pain reduction was not noted (likely due to limited sample size), there was a trend toward improved pain and anxiety outcomes when VR was added to standard analgesia [16]. Importantly, the study advocated the use of inexpensive VR setups to be safe and well-tolerated. They could potentially be implemented in low-resource burn units [16]. Hence, in low- and middle-income countries (LMICs), where conventional rehab resources are scarce; low-cost and consumer-grade VR systems could be adopted for rehabilitation.
Overall, there is a need for more high-quality trials as noted by recent review articles advocating the benefits of VR in rehabilitation. VR-based exercises greatly improve strength, skill, and mobility across conditions. Secondly, users found VR-based therapy more engaging than traditional exercises as highlighted by published reviews [2, 3]. Another review was conducted which focused on neurodegenerative diseases like Parkinson’s, multiple sclerosis. They similarly concluded VR interventions to be effective and well-tolerated, though it called for larger RCTs to confirm long-term benefits [17].
This review employed a narrative synthesis rather than a meta analytic approach, despite providing a comprehensive synthesis. Further, direct comparability and generalization of findings were restricted due to substantial heterogeneity. There is also publication biasness as studies with null or negative findings remain under-represented while those reporting positive outcomes become likely to be published.
CONCLUSION
Virtual reality (VR) is a powerful alternative to the conventional rehabilitation. To recognize the maximum potential of the VR, large scale trials with longer follow-ups and standardized outcome measures should be focused and explored in future researches. In order to improve real world recovery and quality of life for patients with neurological and musculoskeletal conditions; advances like VR-based rehab could become a routine, evidence-based option.
DECLARATIONS & STATEMENTS
Author’s Contribution
SG, AS and KB: substantial contributions to the conception and design of the study.
SG, AS: acquisition of data for the study.
AS and KB: interpretation of data for the study.
IA, RAB and KB: analysis of the data for the study.
SG and KB: drafted the work.
SG, AS and KB: revised it critically for important intellectual content.
SG, AS and KB: final approval of the version to be published and agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All authors contributed to the article and approved the submitted version.
Ethical Statement
This narrative review uses only published literature and involves no human or animal subjects; therefore, no ethical approval or consent was required. All sources were appropriately cited and ethical standards were followed.
AI Use Statement
The authors used Grammarly to improve language clarity during manuscript preparation. All final content was reviewed and approved by the authors.
Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data presented in this study are available on request from the corresponding author.
Acknowledgments
None to declare.
Funding Sources
None to declare.
Conflicts of Interest
None to declare.
REFERNCES
Created with Word to HTML Converter- Fu W, Ji C. Application and effect of virtual reality technology in motor skill intervention for individuals with developmental disabilities: A systematic review. Int J Environ Res Public Health. 2023;20(5):4619. [CrossRef] [PubMed]
- Capriotti A, Moret S, Del Bello E, Federici A, Lucertini F. Virtual reality: A new frontier of physical rehabilitation. Sensors. 2025;25(10):3080. [CrossRef] [PubMed]
- Cardile D, Arena C, Corallo F, Giuffrida GM, Giustiniani A, Maggio MG, et al. A systematic review on the use of virtual reality in post-stroke patients: Exploring when modalities make the difference in executive and motor recovery. Frontiers in Virtual Reality. 2025;Volume 6 - 2025. [CrossRef]
- Garofano M, Del Sorbo R, Calabrese M, Giordano M, Di Palo MP, Bartolomeo M, et al. Remote rehabilitation and virtual reality interventions using motion sensors for chronic low back pain: A systematic review of biomechanical, pain, quality of life, and adherence outcomes. Technologies. 2025;13(5):186. [CrossRef]
- De Natale G, Qorri E, Todri J, Lena O. Impact of virtual reality alone and in combination with conventional therapy on balance in Parkinson’s disease: A systematic review with a meta-analysis of randomized controlled trials. Medicina. 2025;61(3):524. [CrossRef] [PubMed]
- Demeco A, Zola L, Frizziero A, Martini C, Palumbo A, Foresti R, et al. Immersive virtual reality in post-stroke rehabilitation: A systematic review. Sensors. 2023;23(3):1712. [CrossRef] [PubMed]
- Fang E, Guan H, Du B, Ma X, Ma L. Effectiveness of virtual reality for functional disorders in cerebral palsy: An overview of systematic reviews and meta-analyses. Front Neurol. 2025;Volume 16 - 2025. [CrossRef] [PubMed]
- Wei X, Huang C, Ding X, Zhou Z, Zhang Y, Feng X, et al. Effect of virtual reality training on dual-task performance in older adults: A systematic review and meta-analysis. J Neuroeng Rehabil . 2025;22(1):141. [CrossRef] [PubMed]
- Elser A, Ohse M, Frankenstein C, Leeuw M, Schiebler S, Schmieder S, et al. Usage of virtual reality technology in physiotherapy in Germany: Results from a survey. Bioengineering. 2025;12(2):106. [CrossRef] [PubMed]
- Zhang J, Liu M, Yue J, Yang J, Xiao Y, Yang J, et al. Effects of virtual reality with different modalities on upper limb recovery: A systematic review and network meta-analysis on optimizing stroke rehabilitation. Front Neurol. 2025;16:1544135. [CrossRef] [PubMed]
- Tobaiqi MA, Albadawi EA, Fadlalmola HA, Albadrani MS. Application of virtual reality-assisted exergaming on the rehabilitation of children with cerebral palsy: A systematic review and meta-analysis. J Clin Med. 2023;12(22). [CrossRef] [PubMed]
- Zak M, Sikorski T, Michalska A, Sztandera P, Szczepanowska-Wolowiec B, Brola W, et al. The effects of physiotherapy programmes, aided by virtual reality solutions, on balance in older women: A randomised controlled trial. J Clin Med. 2024;13(21). [CrossRef] [PubMed]
- Banikova S, Najsrova A, Szegedi I, Vitova K, Fiedorova I, Trda J, et al. Patient satisfaction and tolerance of virtual reality rehabilitation in subacute ischemic stroke: A pilot study. Front Rehabil Sci. 2025;6:1660766. [CrossRef] [PubMed]
- Mesa-Burbano AE, Fernández-Polo MA, Hurtado-Sánchez JS, Betancur-Bedoya SP, Quiguanas-López DM, Ordoñez-Mora LT. Effects of virtual reality use on children with cerebral palsy and its applications in health: A systematic review. Healthcare (Basel). 2025;13(20). [CrossRef]
- Slatman S, Staal JB, van Goor H, Ostelo R, Soer R, Knoop J. Limited use of virtual reality in primary care physiotherapy for patients with chronic pain. BMC Musculoskelet Disord. 2024;25(1):168. [CrossRef] [PubMed]
- Morris LD, Louw QA, Crous LC. Feasibility and potential effect of a low-cost virtual reality system on reducing pain and anxiety in adult burn injury patients during physiotherapy in a developing country. Burns. 2010;36(5):659-64. [CrossRef] [PubMed]
- Solares L, Llana T, García-Navarra S, Mendez M. Advances in virtual reality-based physical rehabilitation for neurodegenerative diseases: A systematic review. Applied Sciences. 2025;15(18):9903. [CrossRef]
- Lu W, Shi M, Liu L, Wang S, Deng W, Ma Y, et al. Effect of virtual reality-based therapies on lower limb functional recovery in stroke survivors: Systematic review and meta-analysis. J Med Internet Res. 2025;27:e72364. [CrossRef] [PubMed]
Submitted
Accepted
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Samina Ghulam, Amjad Sharif, Komal Bhatti

This work is licensed under a Creative Commons Attribution 4.0 International License.
Authors retain copyright and grant the journal right of first publication and allows others to share the work with an acknowledgment of the work’s authorship and initial publication in this journal. No use, distribution or reproduction is permitted which does not comply with these terms.