Vibroacoustic Therapy in Neurorehabilitation: Emerging Potential and Gaps
DOI:
https://doi.org/10.52567/trehabj.v9i04.111Keywords:
Vibroacoustic Therapy, Neurorehabilitation, Cerebral Palsy, Stroke Rehabilitation, Spasticity, Home-Based Rehabilitation, Motor Function Recovery, Sensory Stimulation, Non-Invasive Therapy, Music TherapyAbstract
Background: Vibroacoustic therapy (VAT) employs low-frequency sound vibrations in combination with therapeutic interventions to enhance neuromotor rehabilitation. It is increasingly explored for managing symptoms associated with neurological disorders such as cerebral palsy (CP), stroke, and multiple sclerosis (MS), including spasticity, proprioception, and neuroplasticity.
Objective: This review summarizes current evidence on VAT in neurorehabilitation, highlights its mechanisms of action, discusses clinical applications, and outlines future challenges and directions.
Methods: Relevant literature on VAT, including randomized controlled trials, quasi-experimental studies, and systematic reviews, was synthesized to evaluate its therapeutic potential, feasibility, and emerging applications.
Results: VAT uniquely integrates mechanical oscillations with music, distinguishing it from conventional vibration therapies. Evidence supports its benefits in reducing spasticity, enhancing motor recovery, and improving sensory function in both paediatric and adult populations. VAT also shows promise in respiratory conditions and in home-based care using wearable technology. Despite its potential, VAT research remains limited, underfunded, and hindered by a lack of standardized treatment protocols.
Conclusion: VAT holds promise as a safe, non-invasive adjunct to conventional rehabilitation, particularly for CP and stroke. Standardization of protocols and large-scale clinical trials are required before widespread clinical adoption can be recommended.
INTRODUCTION
Vibroacoustic therapy (VPT), initially designed by Olav Skille in the 1980s, following the groundwork laid by Teirich in the late 1950s, who examined the potential of combining music and vibrations [1]. It involves transmitting Low-frequency auditory vibrations, typically not exceeding 100 Hz, through the body using devices embedded in household items such as mats, chairs, or wearable devices. Muscle tone and neural excitability are thought to be influenced by these vibrations, along with psychological states, by stimulating mechanoreceptors and modulating the nervous system [2,3].
A key difference between VAT and other vibratory interventions, such as Whole-Body Vibration (WBV), is that they rely solely on mechanical vibration, whereas VAT uses mechanical sound vibrations along with music therapy to promote greater clinical benefits and accelerate the rehabilitation process [4]. In the context of neuro-physiotherapy, VAT aims to augment conventional therapies through enhancing motor outcomes and reducing spasticity, making it a subject of growing interest in paediatric and adult rehabilitation.
MECHANISMS OF ACTION
The proposed mechanisms behind VAT's therapeutic benefits are multifaceted. Vibratory stimulation may potentially enhance the flow of cerebrospinal fluid and accelerate the clearance of metabolic waste. One central mechanism is thought to be neuromodulation through mechanical oscillation, where sound waves activate skin and muscle mechanoreceptors, specifically, and the Pacinian corpuscles. These are known for their pain modulation properties and tactile, along with vibratory perception activity, and respond to a wide frequency range of 60 to 600 Hz, causing decreased excitability in reflex pathways of spastic muscles. These effects are believed to modulate afferent inputs and amplify the activity of inhibitory interneurons, potentially reducing hypertonia and causing muscular relaxation due to a resonance response [5,6]. VAT is also thought to facilitate neuroplasticity. Studies have suggested that vibrations at 100 Hz can trigger adaptive changes within neural circuits in the brain and the spinal cord and support motor learning, and are also capable of activating the mechanoreceptors [7].
In addition, VAT offers notable musculoskeletal advantages, such as reducing muscle pain by improving blood flow. The rhythmic stimulation may support more accurate proprioceptive signalling and promote coordinated voluntary movements, especially when used alongside conventional physical therapy. However, further research is necessary, as to date, no empirical biological data support the hypothesis that blood circulation improves with VAT [8]. Figure 1 summarizes the mechanisms of action of VAT.
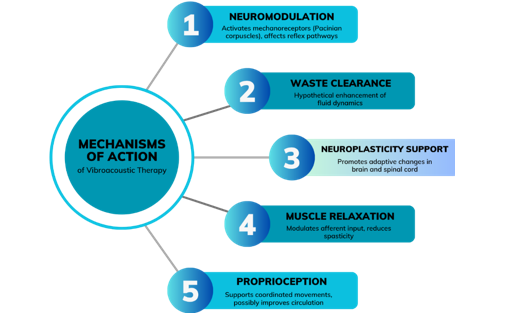
Figure 1: Mechanisms of Vibroacoustic Therapy
APPLICATIONS IN CEREBRAL PALSY (CP)
Existing evidence from RCTs and quasi-experimental studies has evaluated the effectiveness of VAT in children with spastic CP and reported meaningful improvements in motor control, spasticity reduction, along with functional mobility. A landmark study by Alena Adaikina et al. consisted of 34 children within the age range of 6.0 to 12.6 years with a diagnosis of CP undergoing a 20-week VAT protocol in conjunction with conventional therapy.
Results demonstrated significant enhancements in GMFM scores and reduced lower-limb spasticity compared to controls [9].
In another study, Liu et al. combined VAT with traditional Chinese music and applied it to 90 children with spastic CP. Among participants receiving physiotherapy alone, with music, or with VAT, beneficial effects were evident exclusively in the VAT group, as evident by significant reductions in muscle tone and improved joint mobility [10]. These findings emphasize the additional therapeutic advantage of mechanical vibration compared to auditory stimulation alone.
Zahra Ahmadizadeh et al. conducted a trial using whole-body vibration (WBV), a related form of VAT, alongside passive stretching for children with CP. Over six weeks, participants exhibited improvements in Ashworth scores, muscle strength, and postural balance [11]. Long-term effects of VAT have also been assessed. Fatih Tekin et al. conducted an 8-week study. 22 children with CP were allocated into 2 groups. The intervention group receiving WBV reported enhancements in walking speed and motor coordination, along with reduced spasticity in the treatment group, and the effects were preserved even after 12 weeks as compared to the control group receiving conventional therapy [12]. These outcomes suggest that extended application of vibration-based therapies may result in sustained motor gains. However, there is limited literature and research on the long-term benefits of VAT in CP children, but the benefits of WBV suggest that the gains obtained from VAT will be similar. This calls for large-scale RCTs to gain insights into the effects of VAT.
STROKE REHABILITATION AND ADULT APPLICATIONS
Although most research on VAT has focused on paediatric CP, its application in adult neurorehabilitation, particularly stroke, is expanding. A notable feasibility trial by Seim et al. investigated a wearable vibrotactile stimulation (VTS) glove for chronic stroke survivors. Participants experienced improved sensory feedback, reduced upper-limb spasticity, and a greater range of motion following regular use of the glove [13]. This supports VAT's relevance for upper-limb rehabilitation post-stroke and highlights the potential of integrating wearable technology into therapy protocols.
Furthermore, to evaluate the effect of VAT on Depression and Cognitive Disorders in People Living with Stroke, a 2025 systematic review revealed significant upper-limb strength and range-of-motion gains following treatment, along with improvement in depression and cognitive function [14]. Although the majority of research is conducted in a podiatric population, its implications for adult stroke patients are worth exploring due to similarities in motor deficits and rehabilitation goals.
FEASIBILITY AND HOME-BASED APPLICATIONS
VAT’s non-invasive and adaptable nature makes it particularly suitable for home-based interventions as well. Campbell et al. used a mixed-methods approach to evaluate a two-phase intervention (Phase I: Professional-Led Sessions, Phase II: Self-Care with Technology) and concluded that the self-care component was found to meaningfully support ongoing recovery, especially in managing milder symptoms and preserving treatment efficacy across non-intensive periods [4]. No adverse effects were observed, reinforcing VAT’s safety profile and feasibility outside clinical settings. Figure 2 provides an overview of VAT applications within neurorehabilitation.
FUTURE DIRECTIONS
VAT research is hindered by several limitations. Variation in treatment protocols is a major issue because studies vary in frequency, duration, session frequency, and whether music is included. This diversity reduces the reliability of aggregated data and its applicability. Additionally, many trials lack blinding or use subjective outcome measures, which can introduce bias.
Future research should prioritize standardizing VAT protocols to determine optimal frequencies, session durations, and treatment schedules. Evidence suggests that VAT is beneficial in patients with CP or stroke to treat clinical manifestations such as impaired sensation and spasticity; however, there are no accurate treatment protocols or parameters, such as frequency, time, and intensity, defined for using the VAT to gain beneficial effects as reported in a scoping review conducted by Kantor J et al [4]. Larger, multicentre RCTs should determine these parameters to set an authentic treatment protocol. This will not only be a step towards the advancement in the field of treating secondary complications related to CP or stroke, but will also help therapists globally to use VAT efficiently without causing adverse effects. RCTs should also examine not only motor outcomes but also functional independence, caregiver burden, and cost-effectiveness.
Developing consensus guidelines would support clinical implementation and trial reproducibility. Furthermore, extending VAT research beyond CP and stroke to populations with MS, traumatic brain injury (TBI), and Parkinson’s disease is warranted. These conditions share characteristics like impaired sensorimotor integration and spasticity, for which VAT may offer benefits. Apart from neurological problems, VAT can also be beneficial in patients with respiratory disorders such as COPD, Pneumonia, and acute respiratory distress syndrome (ARDS), as reported by Aidos Konkayev in a clinical trial about the effects of VAT in patients with COVID-19 complicated by respiratory failure [15]. Therefore, this emphasizes the need for further research and larger-scale RCTs to gain insight into either beneficial or adverse effects of VAT in patients with respiratory complications and to determine the mechanism of action in treating its symptoms if proven to be beneficial.
Another emerging area of interest is the integration of VAT as a parallel intervention to conventional therapy, especially for children with cerebral palsy or individuals with autism, where behavioural regulation during the delivery of intervention can often be challenging. As noted by Marko Punkanen and Esa Ala-Ruona [3], music therapy may serve as a component of VAT. Thus, incorporating soothing and mind-relaxing background music during VAT sessions could help calm autistic individuals, potentially enhancing the effectiveness of conventional therapy and gaining the beneficial effects offered by VAD as an addition. However, further research is necessary to determine the potential and therapeutic value of this combined approach.
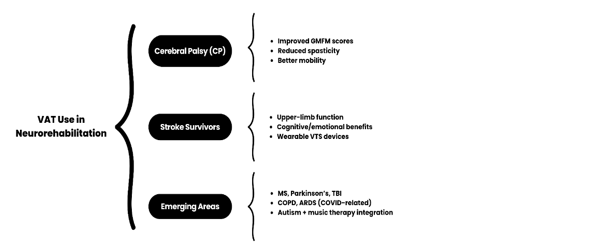
Figure 2: Clinical uses of vibroacoustic therapy across neurological and emerging rehabilitation contexts.
Finally, innovations in wearable Vibroacoustic devices and mobile app-controlled therapy platforms could revolutionize how VAT is delivered, making it a vital component of rehabilitation strategies.
CONCLUSION
Vibroacoustic therapy holds significant promise as an adjunct in neuro-physiotherapy. Its application in cerebral palsy and stroke has shown encouraging outcomes in reducing spasticity and enhancing motor function. Although evidence supports its safety and efficacy, after reviewing the available evidence on VAT’s effects on muscle function and tone, it can be concluded that extensive investigation is needed before physicians and therapists can utilize this therapy as a routine part of clinical neurological practice or in senior nursing homes. With the growing emphasis on non-invasive, patient-centred, and home-based rehabilitation tools, VAT stands as a promising adjunct in the advancement and evolution of neurorehabilitation. Currently, VAT is not recognized as a potential intervention by the majority of healthcare programs, because this novel therapy lacks sufficient evidence published in medical literature.
DECLARATIONS & STATEMENTS
Author’s Contribution
The following format should be used for author’s contribution.
MUA: substantial contributions to the conception and design of the study.
HA and UNG: acquisition of data for the study.
UNG and HM: interpretation of data for the study.
MUA and HM: analysis of the data for the study.
MUA, HA, UNG and HM: drafted the work.
MUA, HA, UNG and HM: revised it critically for important intellectual content.
MUA, HA, UNG and HM: final approval of the version to be published and agreement to be accountable for all aspects.
of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All authors contributed to the article and approved the submitted version.
Ethical Statement
This narrative review uses only published literature and involves no human or animal subjects; therefore, no ethical approval or consent was required. All sources were appropriately cited and ethical standards were followed.
AI Use Statement
The authors used Grammarly to improve language clarity during manuscript preparation. Generative AI tools such as ScisSpace and Semantic Scholar were used to assist with literature summarization and refinement of the research rationale. All interpretations, conclusions, and original ideas remain solely those of the authors and approved by the authors.
Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data presented in this study are available on request from the corresponding author.
Acknowledgments
None to declare.
Funding Sources
None to declare.
Conflicts of Interest
None to declare.
REFERENCES
Professional Email Signature- Ala-Ruona E, Punkanen M, Campbell E. Vibroacoustic therapy: Conception, development, and future directions. Musiikkiterapia. 2015;30(1-2):48-71.
- Kantor J, Kantorová L, Marečková J, Peng D, Vilímek Z. Potential of vibroacoustic therapy in persons with cerebral palsy: an advanced narrative review. Int J Environ Res Public Health. 2019 Oct 16;16(20):3940. [CrossRef] [PubMed]
- Punkanen M, Ala-Ruona E. Contemporary vibroacoustic therapy: perspectives on clinical practice, research, and training. Music Med. 2012 ;4(3):128–135. [CrossRef]
- Kantor J, Campbell EA, Kantorová L, Marečková J, Regec V, Karasová K, Sedláčková D, Klugar M. Exploring vibroacoustic therapy in adults experiencing pain: a scoping review. BMJ Open. 2022 Apr 5;12(4):e046591. [CrossRef] [PubMed]
- Bartel L, Mosabbir A. Possible Mechanisms for the Effects of Sound Vibration on Human Health. Healthcare (Basel). 2021 May 18;9(5):597. [CrossRef] [PubMed]
- Barassi G, Pellegrino R, Matera GL, Prosperi L, Younes A, Guglielmi V, Cuozzo M, Parone C, Di Iorio A, Panunzio M. Integrated approach in chronic pain from musculoskeletal stiffness: music therapy and vibro-acoustic platform. Eur J Musculoskel Dis. 2024 Sep;13(3):11-7.
- Viganò A, Celletti C, Giuliani G, Jannini TB, Marenco F, Maestrini I, Zumpano R, Vicenzini E, Altieri M, Camerota F, et al. Focal muscle vibration (FMV) for post-stroke motor recovery: multisite neuroplasticity induction, timing of intervention, clinical approaches, and prospects from a narrative review. Vibration. 2023; 6(3):645-658. [CrossRef]
- Shah VD. A critique of vibroacoustic therapy for physical and mental ailments. Undergrad J Psychol. 2021.
- Adaikina A, Derraik JGB, Hofman PL, Gusso S. Vibration therapy in young children with mild to moderate cerebral palsy: does frequency and treatment duration matter? A randomised-controlled study. BMC Pediatr. 2023 Jan 2;23(1):4. [CrossRef] [PubMed]
- Liu ZH, Zhang LH, Zhao Y. Effect of vibroacoustic therapy with five elements music on muscle tone of children with cerebral palsy. Chin J Rehabil Theory Pract. 2013;19(8):771–774.
- Ahmadizadeh Z, Khalili M, Ghalam M, Mokhlesin M. Effect of whole body vibration with stretching exercise on active and passive range of motion in lower extremities in children with cerebral palsy: a randomized clinical trial. Iran J Pediatr. 2019 Aug 25. [CrossRef]
- Tekin F, Kavlak E. Short and long-term effects of whole-body vibration on spasticity and motor performance in children with hemiparetic cerebral palsy. Percept Mot Skills. 2021 Jun;128(3):1107-1129. [CrossRef] [PubMed]
- Seim CE, Wolf SL, Starner TE. Wearable vibrotactile stimulation for upper extremity rehabilitation in chronic stroke: clinical feasibility trial using the VTS Glove. J Neuroeng Rehabil. 2021 Jan 23;18(1):14. [CrossRef] [PubMed]
- Wang Z, Xue Y, Sun G, Yun J, Li Y, Chen Q, Wang R, Wang J, Ren C. Effects of Music-Supported therapy for depression and cognitive disorders in people living with stroke and its impact on quality of life: a systematic evaluation and meta-analysis. Cerebrovasc Dis. 2025 Jan 6:1-26. [CrossRef] [PubMed]
- Konkayev A, Bekniyazova A. Vibroacoustic therapy in the treatment of patients with COVID-19 complicated by respiratory failure: a pilot randomized controlled trial. Front Med (Lausanne). 2023 Dec 14;10:1225384. [CrossRef] [PubMed]
Submitted
Accepted
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Muhammad Usman Ali, Haleema Akhtar, Ujala Nauman Ghumman, Muhammad Haseeb

This work is licensed under a Creative Commons Attribution 4.0 International License.
Authors retain copyright and grant the journal right of first publication and allows others to share the work with an acknowledgment of the work’s authorship and initial publication in this journal. No use, distribution or reproduction is permitted which does not comply with these terms.